Interstitial Cystitis
Interstitial Cystitis
About Interstitial Cystitis/Bladder Pain Syndrome
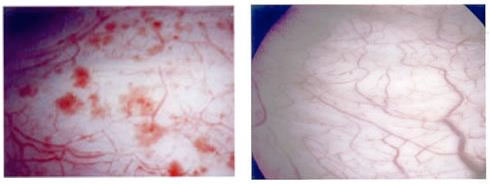
Interstitial Cystitis (IC) is a chronic inflammation of the bladder wall, which can also be diagnosed as Bladder PainSyndrome (BPS). The cause of IC/BPS is not yet known, research continues to find the cause. Indications suggest the condition could be due to a defective bladder lining, or an autoimmune disorder. IC/BPS may resemble a bacterial bladder infection, however short term antibiotics are not effective.
Helpful links
How common is IC/BPS?
BPS /IC is a chronic condition with unknown aetiology (cause of the disease) As the definition of IC/BPS has evolved it is seen now as a diagnosis of exclusion with no definitive diagnostic test; hence it is difficult to estimate prevalence, which can be dependant on whether symptoms are clinician assigned or patient reported. We know from NHS Digital that in 204/15 (last available stats) that there were over 330,000 Patient Episodes (Admissions to Hospital) of Urinary related problems including IC.
Having the right information about your condition is vital.
What are the main symptoms of IC/BPS?
Patients may experience some or all of the following symptoms:
- FREQUENCY - Day and/or night frequency of urination.
- URGENCY - The sensation of having to urinate immediately may also be accompanied by pain, pressure or spasms.
- PAIN - Can be in the abdominal, urethral or vaginal area. Pain is also frequently associated with sexual intercourse
How can IC/BPS affect an individual’s life?
Many IC/BPS patients find that their life revolves around knowing where the nearest toilet is. Therefore, any trip away from home may require thought and planning. Some severe sufferers of IC/BPS can find themselves virtually housebound, which can lead to other problems such as social isolation and depression. Severe tiredness can also occur if the sufferer has to get up repeatedly during the night.
Bladder issues can be seen as ‘socially unacceptable’ conditions, which are not often discussed in public. They are also 'hidden disabilities' which can lead to some sufferers feeling isolated and misunderstood.
Some may also be in constant pain which can affect relationships and work.
A large number of sufferers find that certain foods or drinks, and even clothing can aggravate their condition.
If you would like information on how to support a friend or relative with IC/BPS please click here
I found Bladder Health UK so helpful at this time. I wouldn’t hesitate to recommend them to others.
How is IC/BPS diagnosed?
This is usually via elimination or diagnostic tests such as Urodynamics or Cystoscopy. It can take time to obtain a correct diagnosis as symptoms of IC/BPS can be similar to other conditions for example, Overactive Bladder or Bacterial Cystitis or Chronic UTI. Progress has been made by BHUK in raising awareness of IC/BPS and the importance of finding the correct treatment for the patient.

Coping with IC/BPS
It is important to gain support from your GP and urologist to work together at finding the correct treatment for your symptoms. Learn to manage your flares (bad days) with self help and medication. Reaching out to others who understand what you are experiencing can be of great benefit. You can connect with other via the Bladder Health UK Closed Facebook page or our website forums.
Some lifestyle changes may help you to cope, examples include: relaxation, diet, exercise, clothing and planned travel, all which can help enable you to live positively with IC/BPS.
How can BHUK help you, if you join us?

Members Magazine "Your Bladder Health", published 3 times per year.

An excellent booklet written to provide practical help and advice.

Telephone Advice Line – 0121 702 0820

Telephone contact - with a BHUK Phone-Pal and fellow sufferer.

Comprehensive Resources - fact sheets, DVDs, lending library, Can't Wait Cards and much more.

Message Forums- exchange personal experiences of bladder illness with others.

Social Media sites including Facebook @BladderHealthUK and Twitter #bladdersupport

Area Co-ordinator - providing an opportunity to have personal contact with other sufferers.
Related
 Get involved
Get involved Fundraising
Fundraising Join now
Join now
